05 November 2021: Original Paper
Single-Center Experience with Hepatic Artery Reconstruction During Living Donor Liver Transplantation: Microscope Versus Surgical Loupe
Chang Ho Seo1ABCDEF, Joseph Ahn1AB, Young Kyoung You1AB, Ho Joong Choi1ABCDE*DOI: 10.12659/AOT.933371
Ann Transplant 2021; 26:e933371
Abstract
BACKGROUND: Hepatic artery reconstruction during living donor liver transplantation is a critical step. To perform this risky procedure, a microscope has been used. However, it takes a long time to complete the procedure and it has a long and steep learning curve. Recently, some transplant surgeons have performed the procedure using a surgical loupe. We conducted this study to compare the outcomes after hepatic artery reconstruction using a microscope versus using a surgical loupe.
MATERIAL AND METHODS: We retrospectively reviewed the outcomes of 300 patients at our institution from April 2014 to July 2020. From April 2014 to September 2017 (era 1), hepatic artery reconstruction was performed using a microscope by an experienced plastic surgeon. From September 2017 to the end date (era 2), it was performed using a loupe (×5.0) by an experienced transplantation surgeon.
RESULTS: There was no difference in most perioperative outcomes between the 2 groups, including the major postoperative complications of hepatic artery complications (2/150 versus 2/150, P=1.000), postoperative bleeding (10/150 versus 5/150, P=0.185), and biliary leakage (18/150 versus 13/150, P=0.343). There was a statistically significant difference between the 2 groups in anastomosis time (42.4±11.8 versus 24.2±7.8, P<0.001) and the entire operation time (436.6±83.9 versus 415.3±68.5, P=0.035).
CONCLUSIONS: We suggest that when the surgeon is familiar with a loupe and vascular anastomosis, hepatic artery reconstruction using a surgical loupe is a safe and feasible method with a shorter operation time.
Keywords: Anastomosis, Surgical, Hepatic Artery, Liver Transplantation, Microscopy, Humans, Living Donors, Vascular Surgical Procedures
Background
For end-stage liver disease and unresectable hepatocellular carcinoma, liver transplantation (LT) has been accepted as the treatment of choice (HCC) [1]. Due to a scarcity of deceased donor grafts, the rate of living donor liver transplantation (LDLT) has grown in recent years [2]. However, due to the small size of the hepatic artery, arterial reconstruction in LDLT is technically more challenging than in deceased donor liver transplantation (DDLT). Hepatic artery complication is one of the most severe complications after LDLT [3] and is the most common vascular complication after LDLT, with estimated incidence rates ranging from 2.5% to 11% [4,5]. Several complications related to hepatic artery reconstruction, such as hepatic artery thrombosis (HAT), hepatic artery stenosis, pseudoaneurysm, and hepatic artery dissection, may lead to graft loss and mortality [6]. After transplantation, all collateral vessels are removed from the graft liver, and arterial blood flow is supplied only by the anastomosed hepatic artery. Therefore, hepatic artery reconstruction in LDLT is the most important procedure for the safety of the recipient.
One of the most significant advancements in hepatic artery reconstruction was the development of microsurgical techniques using a microscope, which has greatly reduced the incidence of HAT and significantly increased graft survival [7,8]. In the past, most centers used a surgical microscope during hepatic artery reconstruction due to the small diameter of the hepatic artery [8]. However, the use of a large surgical microscope has several disadvantages. Due to the deep operative field, the respiratory movement of the patient, and the size disparity between the donor and recipient hepatic artery, reconstructing the hepatic artery using a microscope takes a long time [9]. The hepatic artery reconstruction field is usually 10–15 cm deep from the abdominal wall, making it difficult to visualize the surgical field under a microscope. Furthermore, overcoming the learning curve of microvascular procedures and gaining necessary experience is time-consuming. For this reason, some surgeons suggested that magnification with a surgical loupe could produce comparable outcomes as using a microscope [10]. In the past, hepatic artery reconstruction was done under a microscope at our center, but for the reasons mentioned above, it is currently performed using a surgical loupe. In this retrospective study, we reviewed our experience with hepatic artery reconstruction in LDLT and compared the outcomes between using a microscope versus a surgical loupe.
Material and Methods
STATISTICAL ANALYSIS:
The mean and standard deviation are presented for all numerical data. To compare the continuous variables based on their distribution, the
Results
PATIENT AND PERIOPERATIVE CHARACTERISTICS:
A total of 300 patients who underwent LDLT during the study period were enrolled. The difference between the 2 groups was not statistically significant, except for recipient age, recipient sex, and graft type (right lobe versus left lobe). The mean age of the recipients was 53.99±9.89 (median: 55, 7~77) years and the mean body mass index (BMI) of the recipients was 24.68±3.92. The most common cause of the original liver disease was viral hepatitis-related liver cirrhosis (n=185, 61.6%), followed by alcohol-related liver cirrhosis (n=69, 32.0%). A total of 148 patients were accompanied by HCC (49.3%). The mean Child-Turcotte-Pugh (CTP) and model for end-stage liver disease (MELD) scores were 8.26±2.871 and 16.54±9.886, respectively. A total of 55 patients (18.3%) underwent ABO-incompatible LDLT. There was no statistically significant difference between the 2 groups in pre-transplantation transcatheter arterial chemoembolization (TACE) history or pre-transplantation hepatectomy history, which is considered to be a factor that can induce HAT (Table 1).
OPERATIVE VARIABLES AND SURGICAL OUTCOMES:
Compared to the microscope group, the loupe group showed advantages in anastomosis time (42.47±11.83 versus 24.27±7.83, mean±SD, P<0.001) and the entire operation time (436.66±83.91 versus 415.35±68.55, mean±SD, P=0.035). However, there was no statistically significant difference in ascites, recipient liver weight, estimated blood loss, packed red blood cell (PRC) transfusions, graft fatty change, or hepatic artery size (Table 2).
There was no statistically significant difference in postoperative complications such as postoperative bleeding, hepatic artery complications, biliary strictures, and biliary leaks. There was a total of 15 re-operations, all of which were due to postoperative bleeding. The length of hospital stay, length of ICU stay, and in-hospital mortality showed no statistically significant differences (Table 3).
Discussion
Although LT is the most effective treatment for end-stage liver disease and HCC, it is still considered a high-risk operation with significant morbidity and mortality. LDLT has been established as an alternative to overcome the graft shortage in Asia, where the supply of deceased donors remains below 5 per 1 million population per year [2,11]. However, the surgical procedures for arterial reconstruction in LDLT are more complicated than in DDLT and can cause hepatic arterial complications such as HAT. The introduction of surgical microscope in the 1990s was one of the most significant improvements in hepatic artery reconstruction [8]. Microsurgical techniques overcame the risk of HAT, with an incidence reduced to 1.7% [12].
Although the use of microsurgical techniques in LDLT minimized the problems associated with a high incidence of HAT, it has several disadvantages. First of all, the surgical microscope is bulky and needs to be protected with a sterile plastic bag, which requires additional work. It also requires tricky maneuvering and has difficulties focusing in the abdominal cavity [13]. It offers an operative view at a particular prefixed angle, but time is required to change this setting. Compared to microsurgery on the head, neck, and extremities, it is difficult to make precise observations due to the constant movement of the liver graft in accordance with ventilation. Therefore, ventilation needs to be withheld sometimes during hepatic artery reconstruction using a surgical microscope. For these reasons, some surgeons prefer suturing the artery under a surgical loupe, with more convenient conditions and comparable reported surgical outcomes [14,15].
Postoperative results, including postoperative complications, were comparable between the 2 groups at our center, and the results using a surgical loupe were superior to those of a microscope in terms of operation time and anastomosis time. Other factors such as previous treatment history like TACE or hepatectomy or the size of the hepatic artery can also affect the postoperative outcomes including HAT, but there was no statistically significant difference between the 2 groups. The difference in the incidence by graft type was mainly due to the chronological nature of the 2 groups. As the experience of our center increased, the use of the left lobe became more frequent. The difference in the ratio between the 2 groups may have caused selection bias, but there are several reports that suggest similar postoperative outcomes including HAT between LDLT using the left and right lobes [16–18].
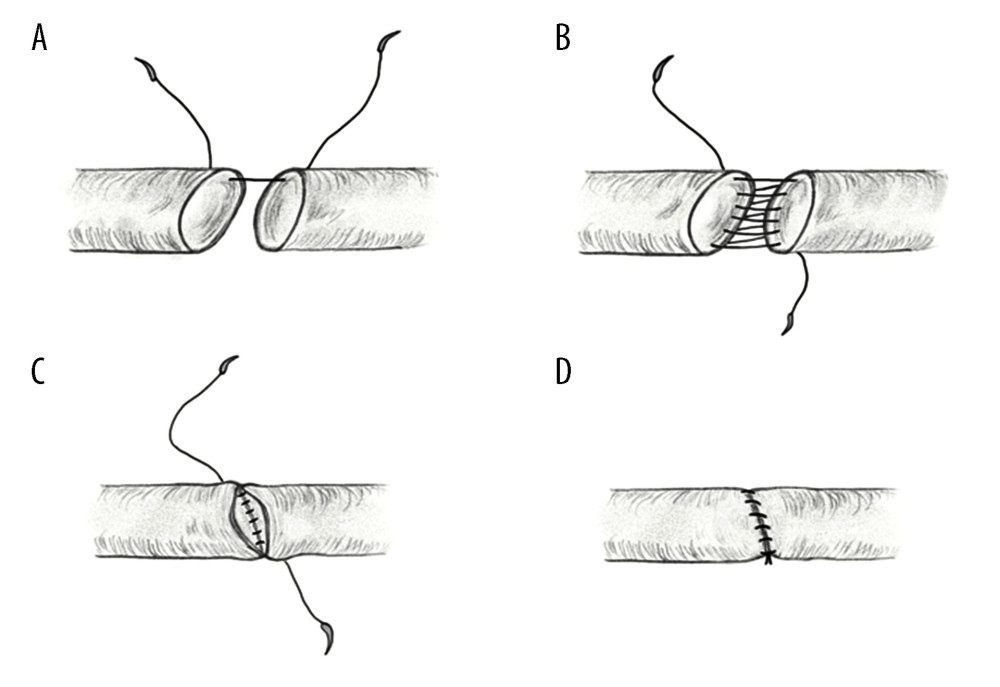
Although hepatic artery reconstruction in a continuous fashion is less time-consuming, there is a concern that it can cause hepatic artery stenosis. However, if there is no hepatic artery dissection and the size of the hepatic artery is not too small (<2 mm), the continuous fashion showed results similar to those of the interrupted fashion [19], consistent with the results in our center. Since we start using a loupe for hepatic artery reconstruction, we usually do reconstruction using continuous fashion. However, when the size of hepatic artery from the graft liver was small, especially when the size discrepancy between the graft and recipient hepatic artery is considerable, we choose an interrupted fashion. Most of the complications related to the hepatic artery are due to surgical factors such as kinking or the wrong axis, but these complications are thought to be irrelevant to whether the method is continuous or interrupted.
In this study, the postoperative outcomes between the 2 groups were not significantly different. However, there were 2 cases of postoperative complications related to the hepatic artery in each group. In our center, re-operation was done when HAT occurred within 1 week after surgery, and interventions were performed when HAT occurred after 1 week. The first case was hepatic artery occlusion, which was detected on postoperative day (POD) 14 by a routine follow-up CT. We inserted a stent via radiologic intervention and the hepatic artery was successfully recanalized. The second case was hepatic artery bleeding with a pseudoaneurysm on POD 9. We tried embolization with intervention, but it failed. We performed a re-operation, and the bleeding was successfully controlled. The third case was HAT on POD 13. We performed an intervention, but it failed. The patient was in poor condition and eventually died. The fourth case was HAT, which occurred on POD 3 but the condition of the graft artery was so poor that it was not possible to perform a re-operation or intervention. Fortunately, despite the poor condition of the hepatic artery, the patient’s condition and LFT were relatively stable, and the hepatic artery was partially recanalized after 6 months using acetylsalicylic acid.
Because hepatic artery complications can cause serious problems in LDLT, hepatic artery reconstruction is one of the most important procedures. Since research reported that hepatic artery anastomosis using a microscope dramatically lowers hepatic artery-related complications [20], the microscope method has been regarded as a standard technique in most LDLT centers. There have been several studies comparing use of the microscope and loupe for microvascular anastomosis, but it is also argued that the difference in the manner of anastomosis whether microscope or loupe is used is insignificant, since both can use the same method of magnification [21]. However, most centers still prefer the microscope method over the loupe method, despite the disadvantage of the microscope method, which requires additional training [22]. In our study, the loupe method had comparable postoperative results to the microscope method and had shorter anastomosis time and operation time. This may be another advantage of the loupe method, as previous studies reported that a prolonged operation time can increase postoperative complications [23,24]. In addition, reduced operating time can minimize surgeon fatigue and enhance the surgeon’s focus on the operation.
This study had some limitations. First, this was a single-center retrospective study, so our results may not be applicable to other centers and some significant biases may have affected the selection of the controls. Due to the retrospective design, data on some operative factors such as the status of the hepatic artery intima or the number of hepatic artery revisions were not collected properly. However, in this study, the microscope method and the loupe method were each performed by a single surgeon who was familiar with the technique, so it seems that the surgeon-related factors were controlled.
Conclusions
This study shows that there was no significant difference in most perioperative outcomes between the microscope group and the loupe group. Therefore, we suggest that when the surgeon is familiar with a loupe and vascular anastomosis, hepatic artery reconstruction using a surgical loupe will be a safe and feasible method with a shorter operation time.
References
1. , Consensus conference: Indications for Liver Transplantation, January 19 and 20 2005. Lyon-Palais Des Congrès: Text of recommendations (long version): Liver Transpl, 2006; 12; 998-1011
2. Chen CL, Fan ST, Lee SG, Living-donor liver transplantation: 12 years of experience in Asia: Transplantation, 2003; 75; S6-11
3. Choi HJ, Kim DG, Kim Y, Clinical course of hepatic artery thrombosis after living donor liver transplantation using the right lobe: Liver Transpl, 2018; 24; 1554-60
4. Proposito D, Loinaz Segurola C, Garcia Garcìa IAssessment of risk factors in the incidence of hepatic artery thrombosis in a consecutive series of 687 liver transplantations: Ann Ital Chir, 2001; 72; 187-205 [in Italian]
5. Stange BJ, Glanemann M, Nuessler NC, Hepatic artery thrombosis after adult liver transplantation: Liver Transpl, 2003; 9; 612-20
6. Ma L, Chen K, Lu Q, Case report of hepatic artery dissection secondary to hepatic artery pseudoaneurysm after living donor liver transplantation: BMC Gastroenterol, 2016; 16; 44
7. Uchiyama H, Hashimoto K, Hiroshige S, Hepatic artery reconstruction in living-donor liver transplantation: A review of its techniques and complications: Surgery, 2002; 131; S200-4
8. Tanaka K, Uemoto S, Tokunaga Y, Surgical techniques and innovations in living related liver transplantation: Ann Surg, 1993; 217; 82-91
9. Li PC, Thorat A, Jeng LB, Hepatic artery reconstruction in living donor liver transplantation using surgical loupes: Achieving low rate of hepatic arterial thrombosis in 741 consecutive recipients-tips and tricks to overcome the poor hepatic arterial flow: Liver Transpl, 2017; 23; 887-98
10. Jwa EK, Kim JD, Choi DL, Comparison of hepatic artery reconstruction using surgical loupe and operating microscope during living donor liver transplantation focusing on the beginner’s point: Ann Hepatobiliary Pancreat Surg, 2019; 23; 122-27
11. de Villa VH, Lo CM, Chen CL, Ethics and rationale of living-donor liver transplantation in Asia: Transplantation, 2003; 75; S2-5
12. Inomoto T, Nishizawa F, Sasaki H, Experiences of 120 microsurgical reconstructions of hepatic artery in living related liver transplantation: Surgery, 1996; 119; 20-26
13. Ohdan H, Tashiro H, Ishiyama K, Microsurgical hepatic artery reconstruction during living-donor liver transplantation by using head-mounted surgical binocular system: Transpl Int, 2007; 20; 970-73
14. Testa G, Losanoff JE, Gangemi A, Benedetti E, Excellent outcome using an alternative technique for arterial reconstruction in living-related liver transplant: sphenoid anastomosis: Transpl Int, 2007; 20; 392-94
15. Guarrera JV, Sinha P, Lobritto SJ, Microvascular hepatic artery anastomosis in pediatric segmental liver transplantation: Microscope vs loupe: Transpl Int, 2004; 17; 585-88
16. Bathla L, Vargas LM, Langnas A, Left lobe liver transplants: Surg Clin North Am, 2013; 93; 1325-42
17. Taketomi A, Shirabe K, Toshima T, The long-term outcomes of patients with hepatocellular carcinoma after living donor liver transplantation: A comparison of right and left lobe grafts: Surg Today, 2012; 42; 559-64
18. She WH, Chok KS, Fung JY, Outcomes of right-lobe and left-lobe living-donor liver transplantations using small-for-size grafts: World J Gastroenterol, 2017; 23; 4270-77
19. Tzeng YS, Hsieh CB, Chen SG, Continuous versus interrupted suture for hepatic artery reconstruction using a loupe in living-donor liver transplantation: Ann Transplant, 2011; 16; 12-25
20. Mori K, Nagata I, Yamagata S, The introduction of microvascular surgery to hepatic artery reconstruction in living-donor liver transplantation – its surgical advantages compared with conventional procedures: Transplantation, 1992; 54; 263-68
21. Barin EZ, Tan O, Cinal H, Our experiences on microsurgical anastomosis of hepatic arteries, without thrombosis, in living donor liver transplantations: Turkish Journal of Plastic Surgery, 2020; 28(3); 140-45
22. Balci D, Ahn CS, Hepatic artery reconstruction in living donor liver transplantation: Curr Opin Organ Transplant, 2019; 24; 631-36
23. Gibbons C, Bruce J, Carpenter J, Identification of risk factors by systematic review and development of risk-adjusted models for surgical site infection: Health Technol Assess, 2011; 15(30); 1-156
24. Cheng H, Chen BP, Soleas IM, Prolonged operative duration increases risk of surgical site infections: A systematic review: Surg Infect (Larchmt), 2017; 18; 722-35
Figures
Tables
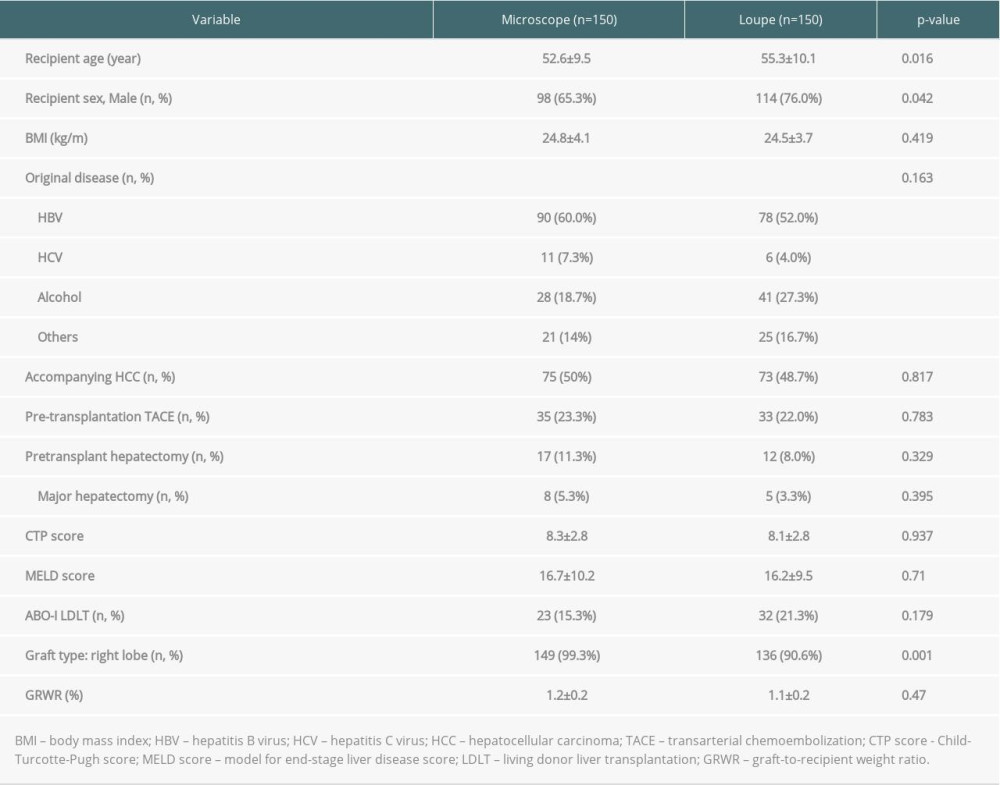 Table 1. Demographic characteristics and preoperative factors of the recipients and donors.
Table 1. Demographic characteristics and preoperative factors of the recipients and donors.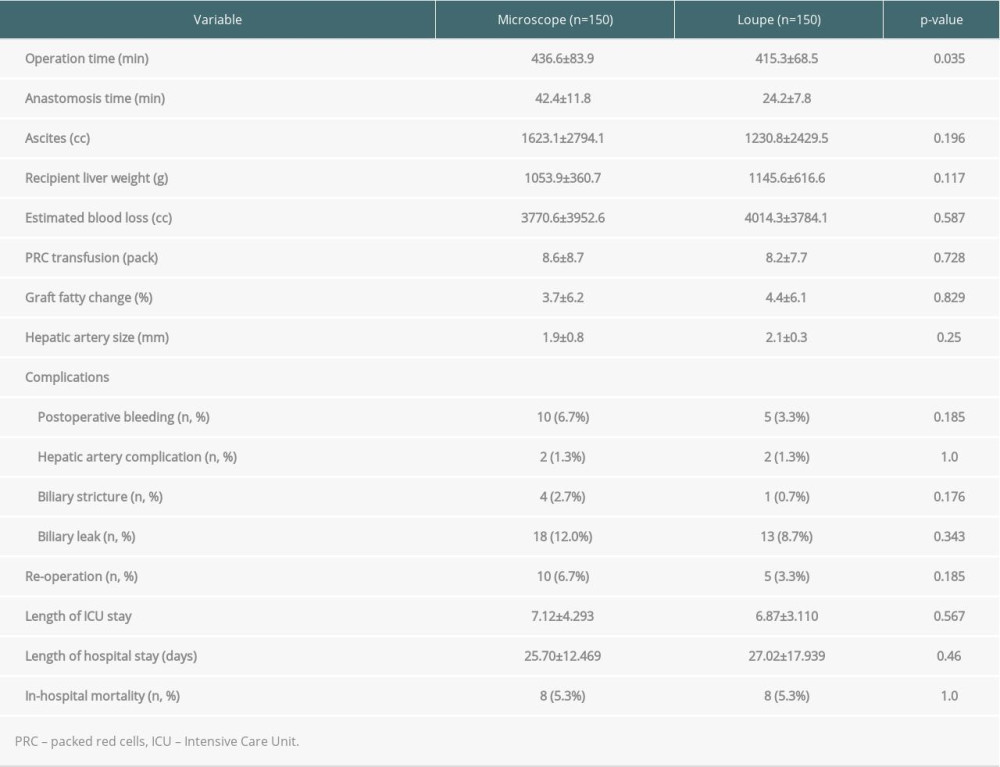 Table 2. Comparison of intraoperative findings and postoperative outcomes.
Table 2. Comparison of intraoperative findings and postoperative outcomes.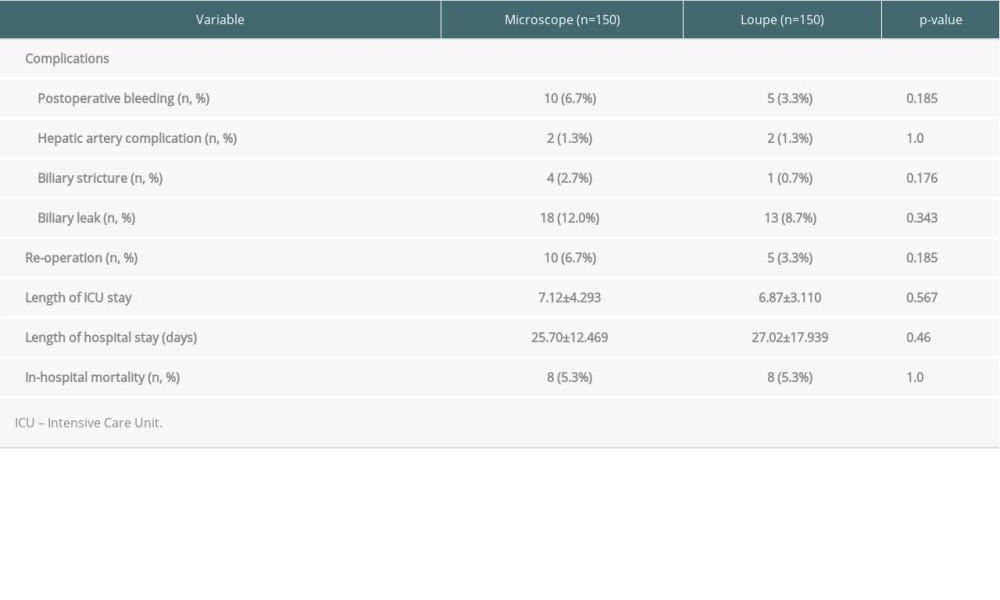 Table 3. Comparison of postoperative outcomes.
Table 3. Comparison of postoperative outcomes. Table 1. Demographic characteristics and preoperative factors of the recipients and donors.
Table 1. Demographic characteristics and preoperative factors of the recipients and donors. Table 2. Comparison of intraoperative findings and postoperative outcomes.
Table 2. Comparison of intraoperative findings and postoperative outcomes. Table 3. Comparison of postoperative outcomes.
Table 3. Comparison of postoperative outcomes. In Press
18 Mar 2024 : Original article
Does Antibiotic Use Increase the Risk of Post-Transplantation Diabetes Mellitus? A Retrospective Study of R...Ann Transplant In Press; DOI: 10.12659/AOT.943282
20 Mar 2024 : Original article
Transplant Nephrectomy: A Comparative Study of Timing and Techniques in a Single InstitutionAnn Transplant In Press; DOI: 10.12659/AOT.942252
28 Mar 2024 : Original article
Association Between FEV₁ Decline Rate and Mortality in Long-Term Follow-Up of a 21-Patient Pilot Clinical T...Ann Transplant In Press; DOI: 10.12659/AOT.942823
02 Apr 2024 : Original article
Liver Transplantation from Brain-Dead Donors with Hepatitis B or C in South Korea: A 2014-2020 Korean Organ...Ann Transplant In Press; DOI: 10.12659/AOT.943588
Most Viewed Current Articles
05 Apr 2022 : Original article
Impact of Statins on Hepatocellular Carcinoma Recurrence After Living-Donor Liver TransplantationDOI :10.12659/AOT.935604
Ann Transplant 2022; 27:e935604
12 Jan 2022 : Original article
Risk Factors for Developing BK Virus-Associated Nephropathy: A Single-Center Retrospective Cohort Study of ...DOI :10.12659/AOT.934738
Ann Transplant 2022; 27:e934738
22 Nov 2022 : Original article
Long-Term Effects of Everolimus-Facilitated Tacrolimus Reduction in Living-Donor Liver Transplant Recipient...DOI :10.12659/AOT.937988
Ann Transplant 2022; 27:e937988
15 Mar 2022 : Case report
Combined Liver, Pancreas-Duodenum, and Kidney Transplantation for Patients with Hepatitis B Cirrhosis, Urem...DOI :10.12659/AOT.935860
Ann Transplant 2022; 27:e935860